|
|
| Reproduction of David Maurice web site at Columbia | [ DavidMaurice.org home page ] |
Columbia University Department of Ophthalmology
presented at ARVO, 1999
| SUMMARY: |
| Usually, studies of the penetration of a drug from the tears to the
retina and vitreous are carried out in the rabbit, somewhat as follows:
Standard Technique
|
| ERRORS IN STANDARD TECHNIQUE |
| 1. Contamination
Tracers of drug from lid margins etc. can spread onto surface of globe during enucleation and then into vitreous. 2. Penetration After Death
|
|
|
| AVOIDANCE OF ERRORS |
1. Small subconjunctival injection This provides a circumscribed zone of high penetration with a border free of drug. 2. Freezing eye after death
|
| EXPERIMENTAL PROCEDURES |
|
| TRACERS | |
| Dyes were used as tracers because their distribution
after injection is visible. Fluorescent dyes can be determined in very
low concentrations.
Rhodamine B (RB) and Sulforhodamine B (RSB) were chosen for representing extremes of lipophilicity. |
|
|
|
|
| INJECTION | |
| A measured volume, ~ 0.2 µl, of 10% SRB or 1% RB injected RE through glass electrode near equator nasal to superior rectus. The solution was made viscous with hyaluronic acid to prevent regurgitation. |
|
| FREEZING | |
| The animal is elevated on a platform.
After death, the right eye is proptosed (A) and dipped into liquid nitrogen (B) for about 1 min. The left eye is then proptosed (C) and both eyes plunged into liquid nitrogen (D) until boiling ceases. |
| PREPARATION OF CORE |
|
| To firmly anchor the frozen head a 1/4 hole is drilled through it
and a bolt is passed through it.
The bolt is fixed in a yoke and attached to the tool post of a hobbyists lathe. A 16 mm diameter channel is bored into the globe with a chilled tool. The core is separated with a saw.
|
| SEPARATION OF TISSUES | |
| The core is lyophilized for 24 hr.
The vitreous can be lifted out cleanly in one piece. The retina comes off in flakes on pressing with a tool. The RPE sometimes comes with it, sometimes not. The choroid is scraped off the sclera. A colored spot is seen centrally on the inside of the sclera of injected eyes. It becomes spread out in the longer term experiments. The sclera can be split form conjunctival tissue. The fluorescent label is extracted from the tissue samples and measured
in a fluorometer that can estimate 1 picogram.
|
| RESULTS |
|
|
Conjunctiva + Sclera |
 |
|
Choroid Rhodamine B |
 |
|
|
 |
|
Choroid Sulforhodamine B |
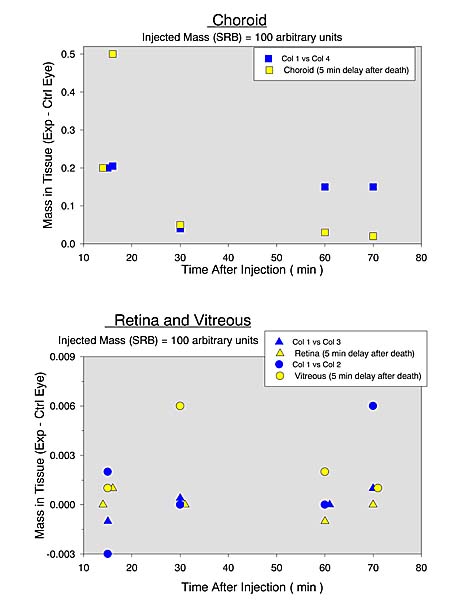 |
| DISCUSSION |
In the choroid it perhaps could be accounted for in part if the tracer accumulated in the stagnant blood in the choroidal vessels and this was squeezed out of the eye during freezing. Further investigation is needed.
|
| CONCLUSIONS |
|
| REFERENCES: |
Supported by NEI and Research to Prevent Blindness
| Reproduction of David Maurice web site at Columbia | [ DavidMaurice.org home page ] |